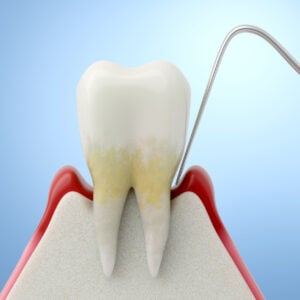
Your mouth is a living ecosystem. Every day your teeth and gums coexist with millions of bacteria, most of which are harmless, and in fact helpful for your oral health. This balanced community is known as the oral microbiome. But when that balance is disrupted, bacteria can trigger inflammation that may escalate into something known as periodontal disease.
What is Periodontal Disease?
Periodontal disease, also known as gum disease, is a group of inflammatory conditions that negatively affect the tissues around the teeth. These supporting structures include:
- Gingiva (gums)
- Periodontal ligament (fibers that suspend the tooth in the socket)
- Alveolar bone (the bone that supports teeth)
The dental specialty focused on gum and bone health is periodontics, and a periodontist is any specialist trained to prevent, diagnose, and treat periodontal disease.
The number one driver of periodontal disease is dental plaque; a sticky bacterial biofilm that forms on teeth and below the gumline. Roughly 42% of all adults over the age of 30 have some form of periodontal disease.
Periodontal Disease Progression
Most people go on to develop gingivitis without consistent oral hygiene. Signs of gingivitis include redness or swelling at the gumline and/or bleeding when brushing or flossing. It’s the earliest stage of gum disease and is typically reversible with better home care and regular, professional cleanings.
As gum disease progresses, bacteria can move into periodontal pockets (spaces between tooth and gum). Once those pockets deepen, plaque and bacteria become harder to remove with brushing and flossing alone.
At most stages, periodontal maintenance in the form of deep cleanings (also known as Scaling and Root Planing or SRP), are required to keep periodontal disease from progressing further. More advanced periodontal disease involves bone loss and increased risk of tooth loss. Periodontitis may progress in “bursts,” with fast active breakdown followed by slow, calm periods.
Signs and Symptoms of Periodontal Disease
Schedule a dental visit if you notice any of the following symptoms (especially if they persist):
- Bleeding gums when brushing or flossing
- Redness or swelling at the gumline
- Persistent bad breath (halitosis) or bad taste
- Gum recession (teeth look “longer”)
- Tooth sensitivity, especially to temperature or pressure
- Periodontal pockets (your dentist measures this during probing)
- Bone loss seen on dental x-rays
- Abscesses (pain, swelling, pus)
Loose or shifting teeth, bite changes, or discomfort chewing
Periodontal Disease Causes and Effects
While periodontal disease begins in the gums, research increasingly points to connections between gum health and overall health. Studies have identified some key risk factors:
- Smoking
- Diabetes
- Heart disease
- Pregnancy complications, such as premature birth and/or low birth weight
If you’re managing chronic health conditions, keeping up with preventive dentistry and periodontal care is an important part of your overall health plan.
How We Diagnose Periodontal Disease
One of the best ways to protect your gums is with regular dental checkups. Our team regularly monitors every patient’s periodontal condition during exams. During a periodontal evaluation, your dentist may:
- Visually examine gum tissues
- Measure gum attachment and pocket depths with periodontal probing
- Review dental X-rays to check bone levels
- Refer you to a periodontist if advanced care is needed
Early diagnosis is key. Catching gum disease early can prevent irreversible bone loss.
Treating Periodontal Disease
Treatment depends on severity, but periodontal care usually includes a combination of home care changes and professional therapy.
Step One: Behavior change
Because plaque drives disease, daily plaque removal matters most. Your dentist may recommend:
- Brushing twice daily with proper technique
- Flossing (or using interdental brushes/water flossers)
- Quitting smoking or vaping
- Improving nutrition and managing risk factors
- A more advanced treatment, such as Perio Defend Therapy custom-fit trays
Consistency is the most important “treatment” for long-term periodontal health.
Step Two: Professional removal of calculus/tartar
Plaque that hardens becomes calculus (also known as tartar) which can’t be removed with home brushing alone.
Scaling and Root Planing removes tartar from above and below the gumline using ultrasonic and hand instruments. Local anesthesia may be used to keep you comfortable during the deep cleaning.
Step Three: Re-evaluation after healing
Your dentist will typically reassess in about 3 to 4 weeks to see how your gums respond. Some patients return to normal gum health with nonsurgical treatment and improved oral hygiene.
Step Four: Bite therapy (when needed)
If issues like clenching/grinding (bruxism) or bite imbalance are contributing to inflammation, bite therapy may be recommended after gum inflammation is under control.
Step Five: Surgical periodontal therapy (for more advanced cases)
If deeper pockets persist, a periodontist may recommend surgery to:
- Reduce pockets
- Regenerate bone/attachment where possible
- Improve gum contours for easier oral hygiene
- Replace missing teeth with options like dental implants (when appropriate)
Key Points
Periodontal disease is able to be treated, and more effectively, prevented altogether with proper diligence. The most effective strategies are still the simplest:
- Maintain excellent oral hygiene by brushing and flossing daily
- Keep up with routine dental cleanings and exams
- Abstain from all smoking and properly manage health conditions like diabetes
- Follow your dentist’s recommended periodontal maintenance schedule if you’ve had gum disease before
Your teeth are meant to last a lifetime, and the key to a long-lasting smile is protecting your gum health.
Ready to Protect your Gum Health?
If you’re noticing bleeding gums, bad breath, gum recession, tooth sensitivity, or it’s simply been a while since your last cleaning; we are here to help! Schedule an appointment online, or call us at (877) 880-1212, to keep your gum health in check and create a personalized plan for a healthy smile for life.
For additional trusted information, visit the American Academy of Periodontology (AAP) and the American Dental Association (ADA).